BMI is an Accurate Predictor of Health: How True is That?

Aditi Shenai
October 19, 2022

Aditi Shenai
October 19, 2022
The body mass index (BMI) is a convenient guide for evaluating a healthy weight range. It takes your height and weight into account to determine whether you are underweight, average weight, overweight, or obese.
BMI is widely used in today’s healthcare settings to flag potential weight-related health issues or to track the chances of obesity. That said, BMI is only a rough guide. There are multiple alternatives to BMI for providing reliable information on how much body fat you are carrying.
Before calculating your BMI value, you should know what BMI is, its calculation, and how the results can affect your health.
Body Mass Index or BMI is a body size measurement concerning your weight and height. The BMI was formulated in 1832 by a Belgian mathematician called Lambert Adolphe Jacques Quetelet.
It is more of an indicator to determine if the weight is healthy and compatible for a particular height. In simple terms, your BMI range estimates your total body fat based on overall weight and size. However, BMI cannot tell you whether your total weight is made up of water, muscle, or fat. As a result, it cannot be used as a diagnostic tool for body fat percentage.
Despite being used since the 1840s, the concept of Body Mass Index has some drawbacks. The first problem is that BMI as a measure is not representative of all demographics. It considered data involving Europeans to determine the range.
Demographics play a role in determining optimum body weight. Also, it does not consider body fat percentage, muscle mass, or body fat distribution, which produces an inaccurate BMI reading. BMI measures cannot distinguish between fat and muscle.
Since muscle tissue is more dense than fat, the density and distribution do not reflect in BMI calculation. For example, the high BMI reading of weight trainers and athletes show as overweight or obese, even when they’re not. Thus, muscular people can be of healthy weight even though their BMI range falls in the obese category.
Another problem is that it doesn’t take into account gender differences. As a result, men and women can have the same BMI readings but different fat percentages.
The body mass index is a simple and inexpensive calculation method using your height and weight. BMI calculators are available online, which give you instant results after entering your age, weight, size, and sometimes, gender.
The study indicates that the BMI scale works on a mathematical formula that infers whether a person is of a healthy weight by halving their weight in kgs by their height in metres squared.
Read More: BMI Calculator – An Informative Outlook on Body Mass Index (BMI)
According to the formula, you get BMI by dividing the weight in kilograms by the square of height in metres. Or the mathematical equation terms are as follows;
BMI = weight (kilogram)/square of the height (m²)
For example, if your weight is 75kg and your height in metres is 1.75, then according to the formula, your BMI will be 24.5.
You can also wield an online BMI calculator, such as the one given by the National Institutes of Health. Once BMI evaluates your weight, it is then correlated to the BMI scale to deduce whether you fall within the “normal” weight span.
In addition to the metric formula, you can also find BMI using the imperial unit formula. You need to divide the weight in pounds by height in inches squared. After that, you should multiply the resulting value by 703 and round it to one decimal place. So, the imperial formula for BMI calculation is:
BMI = weight (lb)/[height (in)]2 x 703
For example, if your weight is 150 pounds and your height in inches is 65, then according to the formula, your BMI will be 24.96.
| BMI Range | Classification | Risk of poor health |
| less than 18.5 | Underweight | High |
| 18.5–24.9 | Normal | Low |
| 25.0–29.9 | Overweight | Low to moderate |
| 30.0–34.9 | Obese class 1 | Moderately (obese) high |
| 35.0–39.9 | Obese class 2 | Severely (obese) very high |
| 40 or greater | Obese class 3 | Extremely (obese) high |
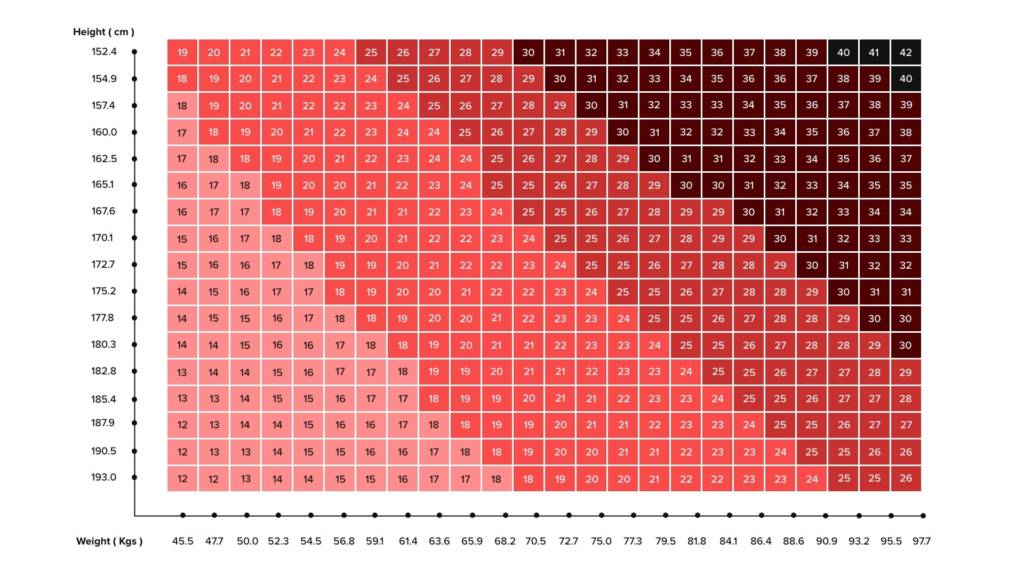
Research indicates that some countries have accepted this BMI scale to illustrate the size and stature of their public in a better way. For example, Asian women and men are at an increased risk of heart disease with a lower BMI, correlated with non-Asians.
Though this can provide the healthcare professional with an image of a person’s health based on their weight, it does not consider other factors such as sex, age, race, fat mass, bone density, genetics, and muscle mass.
Despite the problem that BMI does not accurately specify whether a person is healthy, most research shows that a person’s risk of chronic disease and premature death rises with a BMI less than 18.5 (underweight) or 30.0 or greater (obese).
A 2017 study of 103,218 deaths established that the people who had a BMI of 30.0 or greater (obese) had a 1.5–2.7 times risk of death after a thirty-year follow-up. Another study of 16,868 people indicated that those in the obese BMI category had a 20% increased risk of death from all reasons and heart disease, correlated with those in the normal BMI category.
Other research has shown that a BMI greater than thirty increases the risk of chronic health problems such as heart disease, type 2 diabetes, kidney disease, breathing difficulties, non-alcoholic fatty liver disease, and mobility issues. Furthermore, a study shows a 5-10% reduction in a person’s BMI correlates with decreased rates of heart disease, metabolic syndrome, and type 2 diabetes.
Due to most studies showing a heightened chronic disease risk among people with obesity, many health specialists can use BMI as a common factor of a person’s risk. Still, it should not be the only tool used for diagnosis.
Despite studies correlating a low (below 18.5) and high (30 or greater) BMI with heightened health risks, its use has various flaws.
BMI only answers yes or no, considering whether a person is of average weight, without taking their age, genetics, sex, medical history, lifestyle, or other factors.
Depending only on BMI may omit other significant health measurements, such as blood sugar, blood pressure, cholesterol, heart rate, and inflammation levels, and underestimate or overestimate a person’s proper health.
Finally, solely using BMI to infer a person’s health avoids other facets of health, including mental well-being and mixed up sociological factors such as income, food skills, access to nutritious food, knowledge, and living atmosphere.
Despite studies correlating a low (below 18.5) and high (30 or greater) BMI with heightened health risks, there are various flaws with its use.
Though one pound or kg of muscle weighs the same as one pound or kilograms of fat, muscle is denser and takes up less space. As a result, an individual who is very thin but has high muscle mass may be more prominent on the scale. For example, a two-hundred-pound person who is 5 feet 9 inches tall has a BMI of 29.5, categorising them as overweight.
However, two individuals of the same weight and height could look entirely different. One may have a higher fat mass, and the other may be a bodybuilder with increased muscle mass.
If only BMI is contemplated, this could easily misclassify an individual as overweight or obese despite their low-fat percentage. Therefore, it is significant to evaluate a person’s muscle, bone mass, and fat in addition to their weight.
Though a higher BMI is associated with poorer health consequences, the location of fat on the body may make a more significant discrepancy.
Those with fat stored around their stomach area, apple-shaped or android body types, have a higher risk of chronic disease than those with fat accumulated in their buttocks, hips, and thighs, known as pear-shaped or gynoid body types.
For example, in a survey of 72 studies that comprised data from more than 2.5 million people, investigators found that those with apple-shaped fat percentage had a considerably higher all-cause mortality risk. In comparison, those with a pear-shaped fat percentage had a lower chance.
Medical specialists use their best judgement, implying they would consider the BMI result and consider their patient as an extraordinary individual. However, few health professionals use only BMI to calculate a person’s health before delivering medical recommendations, leading to weight bias and low-quality healthcare.
Those with greater BMIs more frequently report that their doctors concentrate only on their BMI, even if their appointment is for an irrelevant concern. Often, severe medical issues go overlooked as weight-related issues. Studies have indicated that the greater a person’s BMI is, the less likely they are to follow regular health.
Despite the many drawbacks of BMI, it is still used as a fundamental assessment tool because it is cost-effective, convenient, and available in all healthcare settings. However, there are choices to BMI that may be favourable indicators of a person’s health. Each one arrives with its own set of benefits and drawbacks.
Definition: A larger waist circumference, one greater than thirty-five inches in women or forty inches in men, demonstrates more significant body fat in the abdominal area, linked with a higher risk of heart or chronic disease.
Benefits: It is easy to measure, requiring only a measuring tape.
Downsides: It does not evaluate different body types, such as apple-shaped vs pear-shaped, and builds bone and muscle mass.
Definition: A high ratio of 0.95 in men and more significant than 0.80 in women implies higher fat stores in the stomach area and is associated with a higher risk of chronic and heart disease.
As per the World Health Organisation (WHO), a healthy Waist to Hip Ratio is:
Benefits: It is simple to measure and requires only a measuring tape and calculator.
Downsides: It does not evaluate different body types, for example, apple-shaped vs pear-shaped, and builds, for example, bone and muscle mass.
Definition: Body fat percentage is the identical amount of body fat a person has. Some studies indicate that an easy and credible method to evaluate your body fat is to calculate your body’s width from several areas and put that in a formula.
Benefits: It distinguishes between fat-free mass and fat mass and is a more valid representation of fitness risks than BMI.
Downsides: Convenient inspection tools such as skinfold measurements, compact bioelectrical impedance calculation, and at-home scales increase the risk of error.
Definition: Lab tests are numerous blood and essential sign measurements that can demonstrate chronic disease risk—for example, blood pressure, blood glucose levels, heart rate, cholesterol, and inflammation.
Benefits: These tests deliver a more comprehensive review of a person’s metabolic fitness and do not rely only on body fat as a distribution of health.
Downsides: Most of the time, a sole lab value is not adequate to diagnose or demonstrate risk.
Regardless of the inspection tool used, it is essential for healthcare specialists to not depend on one test alone. For example, a healthcare specialist may calculate a person’s BMI and waist circumference, and if a problem arises, a blood test may follow. It is significant to treat each patient as a person to deduce what health means to them mentally, physically, emotionally, and spiritually.
Despite several methods that can help you know whether you have a healthy body weight, it remains unclear which approach is accurate. However, all these methods have undergone enough research to help you analyse your body weight status somehow.
Various detailed studies and the above information shows that excess fat deposition is more dangerous than excess body weight. Hence, it is crucial to focus more on reducing the fat percentage.
You can use these methods as an early indicator to identify whether you need to reduce or gain weight. But, when on a weight loss diet or modified food plan, you should not entirely focus on weight loss. Instead, the focus should be on inch loss. Since visceral fat or abdomen fat is hazardous, inch loss will be a perfect indicator of whether you are on the right track to achieving your fitness goals.
Prioritise a healthy life with optimum body weight, focus on balancing your fat percentage and keeping it to the optimum levels. Set goals for healthy body weight and fat percentage and then decide on modified eating habits. Also, consult an expert nutritionist or health care expert before changing your food plans.
A. BMI is not a precise predictor of health because it does not indicate body fat distribution or body fat percentage. In addition, BMI cannot accurately tell the health of various demographics and races because it was developed with data only containing white Europeans.
A. Waist-to-height ratio (WHtR) is more accurate than BMI because it evaluates central fat. Central fat is significant because it attains around the organs in your abdomen related to ailments such as heart disease.
A. Though people have been using BMI for decades as the go-to measurement for fitness based on body size, studies show it can be wrong to oversimplify what being active means. Many assert not to use BMI in the fitness and medical settings as it is outdated and incorrect.
A. BMI incorporates height and weight, but it does not take sex or age into account. A woman inclines to have more body fat than a man with a similar BMI. Similarly, an older person inclines to have more body fat than a younger person with an identical BMI.
A. Being overweight can result in diseases like high blood pressure, hypertension, High HDL cholesterol, low LDL cholesterol, coronary heart disease, high degrees of triglycerides (Dyslipidemia), and Type 2 diabetes.
A. The study, publicised in the Journal of the American Heart Association, indicates that a waist-to-hip ratio distribution may be an adequate indicator of heart attack risk than BMI (body mass index) for both women and men.
A. Muscle is denser than fat, and an amount of lean mass increases the weight on the scale, which implies you will have an increased BMI. However, because your surplus weight comes from muscle, not additional fat, you won’t have the associated health risks of holding too much body fat.
A. Muscle is denser than fat, and as it is smaller within your body, as you attain muscle mass, you will start looking thinner, no matter your bodily weight. So, if you’ve been doing a lot of strength workouts, it’s likely to be the cause that you are looking great but not dropping those numbers.
A. Body mass index (BMI) is calculated from the height and weight of a person. BMI over twenty-five correlates with higher all-cause mortality and heightened risk of suffering from several diseases, including diabetes and cardiovascular disease.
A.Hip fat location is associated with a higher likelihood of getting type-2 diabetes and heart disease. Your waist-to-hip ratio correlates your hip measurement to your waist measurement. Bigger proportions can mean you have additional fat around your waist, leading to a higher risk for diabetes or heart disease.

